Gingivitis is one of the most common human diseases known and according to studies it affects between 50-90% of the population in the UK/USA. We are sure you agree, that is a significant figure and chances are, you are more than likely to suffer from Gingivitis either now or at some stage in your life. Before we look at how to treat the condition, let us just recap what Gingivitis is and how it is caused:
What is Gingivitis?
Gingivitis literally means inflammation of the gums and its initiating factor is bacteria that live on surfaces of your teeth which are in close proximity to your gums. After you eat, microscopic food particles will cling onto the surfaces on your teeth and bacteria love them. They will use the food particles as an energy source, multiply and start to build entire ecosystems. Dental plaque will start to form within 24 hours if a tooth surface is left undisturbed and that is why it is crucial to brush thoroughly twice daily. The longer the plaque is on your teeth for, the more dangerous they get and the more damage they can do.
How does bacteria cause Gingivitis?
Invasive bacterial species in dental plaque, are able to trick your cell receptors in your gingival tissues and gain entry into your blood stream. The body will realise the gums are now infected and will initiate the inflammatory response to the effort to fight off this infection. The classic inflammatory response can include the following symptoms:
Gingivitis symptoms
- Redness, to increase the blood supply to the area.
- Swelling, for the exudation of fluid.
- Heat. A combination of increased blood flow and release of inflammatory mediators.
- Pain. Pain results from pain receptors picking up on inflammatory exudates and the release of chemical mediators.
- A loss of function, which in advance stages means tooth loss.
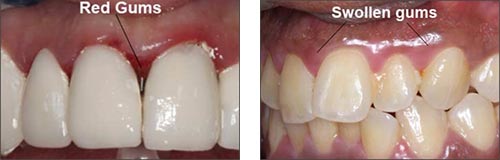
In very advanced gum disease, you will pretty much experience every single one of these signs but in early gum disease you may not experience any pain and therefore, will not necessarily know you have it. So, in relation to gums, this means the typical appearance changes to puffy, red, swollen gums which is much different to the normal appearance of healthy gums which are pink and firm. The images below show what red and swollen gums can look like:
In contrast, this image shows what healthy gums look like:

What happens if you leave Gingivitis untreated?
Gingivitis is the early stage of gum disease; however, it can progress if left untreated. The bacteria will begin to progress below the gum level, and this becomes dangerous because it is very hard for you to access these areas with a normal cleaning routine. Your toothbrush will only be able to reach 1mm or so below the gum, after this the bacteria will be free to multiply without any disturbances. This stage is called periodontitis and its classed as being in the minor stage.
When the bacteria go deep, the gum tissues move away from the teeth creating something called a pocket which allows the bacteria to go even deeper. This stage is referred to as the moderate stage and now the urgency for treatment is much higher. The longer you leave it, treatment will become harder with less chance of a successful outcome. If left at the moderate stage, the bone structures around the tooth will begin to shrink which will lead to the loosening of your teeth.
The next stage, which is classified as severe periodontitis, is when you have had a significant amount of bone loss resulting in a poor long-term outcome for your tooth/teeth. It takes years of neglect for the gum disease to progress this far and it often results in the loss of teeth. In fact, the leading cause of tooth loss in the world is from chronic periodontitis.
How to treat Gingivitis?
If caught early, gum disease does not spread to the supporting structures of the teeth and it is known as a localised inflammatory lesion affecting the gum tissue only. This is super simple to treat and will often resolve within 2 weeks. Treatment involves removing bacterial deposits around the teeth. If there are no hard deposits, known as calculus, regular soft deposits can be removed at home using toothbrushing, floss, interproximal brushes (Like TePe Brushes) and mouthwashes. If there are hard deposits, these are a lot harder to remove at home and you will need to get professional cleaning by your hygienist or dentist. The issue with hard deposits is that they attract soft plaque and allow a rough surface for bacteria to adhere to.
If the gum disease has advanced to periodontitis, whereby the deeper supporting structures of the teeth are affected, then you will definitely need to see a dentist or hygienist to help. If this is the case, our friendly team here at Sensational Smiles would love to advise, why not book an appointment today?